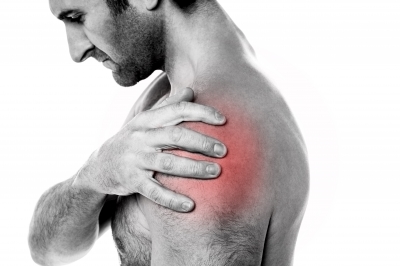
I read an awesome article on TheMighty.com that asked 16 different people on the autism spectrum to describe why making eye contact can be difficult for them. Any insights like this help me be a better parent to my autistic teens and a better educator for emergency responders.
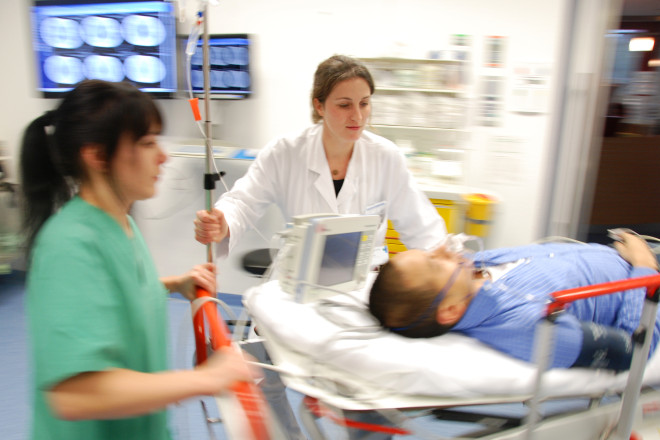
Lack of eye contact may be considered rude or antisocial to those who don’t understand it. However, in an emergency situation that involves first responders, it can be misconstrued as evidence of guilt, non-compliance, or even altered mental status, all of which can put an emergency responder on the defensive and potentially lead to a call going downhill fast.
The Mighty asked their readers with autism who find eye contact difficult to share a description of what it’s like for them. I think some of these quotes are really helpful for emergency responders to be able to understand and identify what’s really going on when someone with autism cannot look at them. The full article can be found here, but some of my favorite descriptions are:
“It’s abstract to me and can be draining. Looking at someone else in the eye means I am taking in everything about them as a person, and I become overloaded. It can disrupt any thought or speaking process I have going on and zaps my energy quickly.” — Laura Spoerl
“To me, eye contact feels like I’m being stared at, like I’m being scrutinized and judged. It makes me uncomfortable because I feel like I’m under immense pressure, and the tension builds and builds until finally I have to look away. It feels almost confrontational, which causes me a lot of anxiety.”— Emma Wozny
“It can feel like you’re standing there naked. It’s very difficult to form a coherent thought with all of this going on in your head. ” — Megan Klein
“When I make eye contact, the world around me blocks out. I can only process the immense pain and discomfort that comes to my brain. This pain goes if I look away.” — Lucy Clapham
“For me it can be a physical pain; it feels like burning with too many emotions, and I just can’t take it in all at once.” — Rosie Howard
“There’s plenty enough for us to concentrate on mid-conversation without the demand to do something which, quite frankly, feels very unnatural to many of us. You can have my eye contact, or you can have my concentration. Choose whichever one you value more.”– Chris Bonnello, from Autistic Not Weird
“Eye contact is hard for me because I am easily overwhelmed by lots of different input. When I am trying to listen, follow, or contribute to a conversation or just manage all my different sensitivities, it is easiest, most comfortable and least painful for me to not make eye contact. I listen and focus better when I am not making eye contact.” — Erin McKinney
My co-trainer at Spirit of Autism, Austin Harris, told me what it’s like for him, and how he’s learned to manage it:
“Eye contact is difficult for me because it makes me very nervous when I’m being looked at directly. It makes me feel uncomfortable in an unexplainable way. One tool I use to combat this is quick contact by looking at multiple people and objects. This works especially well for public speaking and teaching where you need to talk to the group instead of one person. What I do is I make brief contact every so often with different individuals so I am not focusing on just one person’s eyes.”
My daughter shared this with me about her experience:
“If I’m coming up on a person about to pass me, I drop my gaze immediately. If I happen to accidentally lock eyes with them, I feel a tinge of panic. What are they thinking? Are they thinking about me at all? Did I rub them the wrong way? I’d rather be invisible to them, and chances are likely that they thought nothing of it, but I remember it.
There’s something very uncomfortable about looking directly into somebody’s eyes while they’re staring at you. I don’t know what’s going on and I’m trying to evaluate the situation. And how long are you supposed to keep eye contact, anyway? If it’s too short, it may come across as dismissive; if it’s too long, it’s way too awkward. It’s a lot of processing and confusion that goes on underneath the surface in a matter of seconds, and when there are responses and replies expected of you on top of that, it gets to be overwhelming sometimes.”
I think the biggest takeaways for emergency responders when it comes to lack of eye contact are:
- If someone with autism isn’t looking at you directly it does not mean they aren’t listening.
- It can be physically painful for an autistic person to maintain eye contact with you.
- A person with autism may need to avoid eye contact in order to process and focus on what you’re saying to them.
Rather than demanding that someone look at you when you are speaking, it may be helpful to simply ask a person that’s not keeping eye contact with you if they are listening, if they understand you, if they can repeat back what you just said, or even if they’d prefer to communicate by writing.